
HOME > Research
Animal Study I(6):
Kobayashi et al. (1991) fed two groups of animal subjects with either ordinary skim milk (control group) or S100 Milk (treatment group). After seven days’ feeding, the animal subjects were exposed to high doses of X-rays. The animals continued to be fed with ordinary skim milk or S100 Milk until the study concluded. It was found that animal subjects fed with S100 Milk clearly had a higher survival rate than the control group (Fig. 2).
Measurements of IgA production by GALT (Peyer’s patches, mesenteric lymph node) and spleen showed higher levels in the treatment group compared to the control group. In addition, the number of lactobacteria (good bacteria) in the intestinal tract was also shown to increase in the S100 Milk group (Fig. 3).

Fig. 2. Survival Rates of animal subjects after X-rays irradiation shows that survival of treatment group animals was significantly higher than the control group(6).
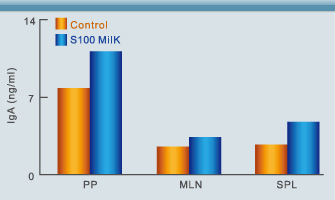
Fig. 3. Measurements of IgA production by Peyer’s patch (PP), mesenteric lymph node (MLN) and spleen (SPL) cells showed that animals fed S100 Milk produced higher levels of IgA compared to the control group(6).
In order to evaluate the potential effects of immune milk products containing specific antibody on the intestinal microflora of cancer patients undergoing chemotherapy treatments, Nomoto et al. (1992) developed an immune milk containing specific antibody against a strain of E. coli commonly found in the mouse GI. Animal subjects were fed either commercial skim milk (Skim-C), commercial WPC (WPC-C) or skim milk containing natural antibodies (Skim-NA) separately as control groups. Separate groups of animals were also fed with whey protein concentrate (WPC) with specific antibody against the mouse strain of E. coli or skim milk with the same specific antibody against the mouse strain of E. coli as the two treatment groups.
After seven days’ feeding, researchers injected the mice with the anti-cancer drug 5-flurouracil (5-FU), inducing side effects similar to what would be expected in similarly treated human subjects (5-FU can cause the number of E. coli in the intestinal tract to increase, resulting in overgrowth and infection). Specific antibodies in the immune milk were shown to effectively prevent E. coli overgrowth in the intestinal tract (Fig. 4 and Table 1). The authors concluded that if patients undergoing long-term chemotherapy were to consume milk containing specific antibodies, the risk of internal infection by E. coli and other bacteria would be effectively reduced or even prevented(7).
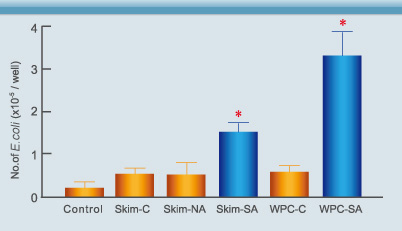
Fig. 4. Shown are the numbers of E. coli phagocytized by macrophages. The treatment groups showed higher levels of phagocytosis than the control groups(7). * p<0.01 Skim-C: Control group (commercial skim milk); Skim-NA: Control group (commercial skim milk containing natural antibody); Skim-SA: treatment group (skim milk containing specific antibody); WPC-C: Control group (commercial WPC); WPC-SA: treatment group (WPC containing specific antibody).
| Days before or after administration of 5-FU | Log10 no.of E.coli in cecum | |||
| Exp | No treatment | Skim-C | Skim-NA | Skim-SA |
| –7 | 3.51±0.74 | 3.51±0.74 | NT | 3.51±0.74 |
| –1 | 3.68±0.57 | 3.34±0.55 | NT | 3.85±0.81 |
| +1 | 8.19±0.57 | 8.00±0.57 | NT | 6.71±1.88** |
| +3 | 8.09±0.24 | NT | NT | 6.39±1.04* |
| +7 | 8.72±0.11 | NT | NT | 8.38±0.28* |
| + 10 | 8.08±0.23 | NT | NT | 8.01±0.27 |
Table 1. E. coli counts in the cecum at times before or after administration of 5-FU. The number of E. coli in the treatment group was significantly lower than the control group(7). NT, not tested. * p < 0.01 and ** p = 0.06
In a study to determine the effects of S100 Milk on aging, Ishida et al. (1992) fed animal subjects with either ordinary skim milk (control group) or S100 Milk (treatment group). After six months’ and after sixteen months’ feeding, animal subjects fed with S100 Milk showed reduced numbers of Enterobacteriaceae in the large intestine and in the cecum (Fig. 5).
In addition, lower serum antibody levels against enteric bacteria suggested that the groups fed S100 Milk had lower levels of invasive bacteria translocating from the intestinal tract into the bloodstream(8) (Fig. 6).

Fig. 5. Determination of the number of enterobacteria in the small intestine, large intestine and cecum, showed that the treatment group had a significantly lower levels than the control group(8). * p<0.01
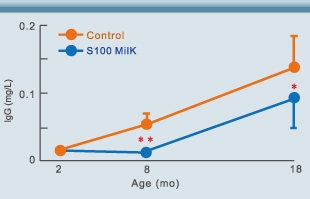
Fig. 6. Measurements of serum antibodies levels against intestinal bacteria show that the treatment group had lower levels than the control group indicating a lower rate of translocation into the bloodstream(8). * p<0.05, ** p<0.01

